Testing & Screening
- Day 3 Bloodwork
- Antral Follicle Count (AFC) & Anti-Mullerian Hormone (AMH)
- Semen Analysis
- Hysterosalpingogram
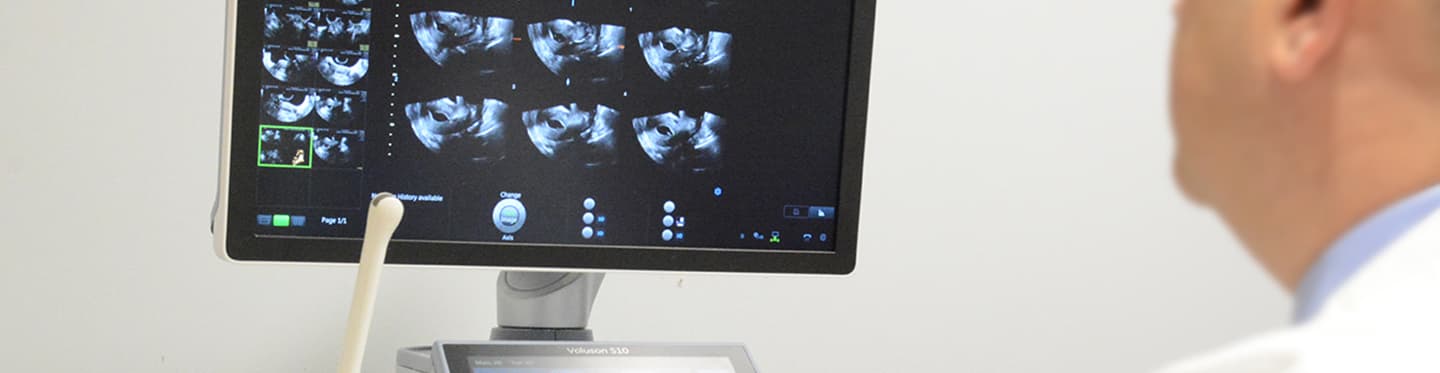
- Transvaginal Ultrasound
- Thyroid Stimulating Hormone (TSH) & Prolactin (PRL)
- General Health & Infectious Disease Screening
- Genetic Screening
- Carrier Screening & Preimplantation Genetic Diagnosis (PGD)
- Preimplantation Genetic Screening (PGS)
Day 3 Bloodwork
 The hormone levels on Day 3 tell us about the communication between the brain and the ovary. Specifically, how hard does the brain need to work to get the ovary to do its job each month.
The hormone levels on Day 3 tell us about the communication between the brain and the ovary. Specifically, how hard does the brain need to work to get the ovary to do its job each month.
As women age, their ovaries become less responsive to the stimulation from the brain. As a result, the brain has to work harder and send more hormone to get the ovary to ovulate. This stimulation happens in the form of a hormone called Follicle Stimulating Hormone (FSH). By checking the hormone levels at the beginning of a cycle, we can get a view into how responsive the ovary is to the messages sent by the brain. The higher the FSH, the harder the brain is working. When the ovary stops responding to the brain’s stimulation entirely, FSH reaches peak levels consistent with menopause.
Antral Follicle Count (AFC) & Anti-Mullerian Hormone (AMH)
 Women are born with all the eggs they will ever have, and with age, the quantity of eggs goes down. Antral Follicle Count (AFC) & Anti-Mullerian Hormone (AMH) are two indirect ways that we can estimate “ovarian reserve” or the amount of eggs remaining in the ovaries.
Women are born with all the eggs they will ever have, and with age, the quantity of eggs goes down. Antral Follicle Count (AFC) & Anti-Mullerian Hormone (AMH) are two indirect ways that we can estimate “ovarian reserve” or the amount of eggs remaining in the ovaries.
Each egg is housed within a tiny fluid filled cyst called a follicle. Many of the follicles are not visible on ultrasound but the one/s that are growing with each cycle and those ready to start growing in a future cycle (antral follicles) can be seen with ultrasound. In addition, each follicle produces a small amount of the hormone AMH. Higher levels of AMH suggest more follicles and lower levels of AMH suggest less follicles. By counting the number of visible antral follicles and testing AMH levels in the bloodstream, we can estimate whether a woman’s quantity of eggs, or ovarian reserve, is in line with her age, increased or diminished compared to other women her age.
Semen Analysis
We will look at the concentration (how many sperm are present in each milliliter of semen), motility (how many of the sperm are moving), and morphology (how many have normal appearance). Men produce millions of sperm in each ejaculate and only a small number are capable of fertilizing an egg. The semen analysis allows us to check if there are enough sperm capable of fertilization in the ejaculate.
Hysterosalpingogram
This study uses an x-ray to check if the tubes are open. Dye is inserted through the cervix into the uterus, if the tubes are open the dye will spill out the ends of tubes. This is visible on the X-Ray. The HSG may also let us know about other abnormalities in the uterus or pelvis.
Transvaginal Ultrasound
An ultrasound allows us to look at the ovaries to count the antral follicles (see above) and look at the uterus. Some abnormalities of the uterus, such as fibroids, may prevent implantation and would be visible on ultrasound.
Thyroid Stimulating Hormone (TSH) & Prolactin (PRL)
Thyroid Stimulating Hormone (TSH) and Prolactin (PRL) are both hormones that may impact the ability to conceive even if you do not have any symptoms. Therefore, these are always included in any initial infertility workup.
General Health & Infectious Disease Screening
In addition to the above testing, we always recommend general health assessment blood work (such as blood count, cholesterol, and others) on the female patient. While these may not interfere with the ability to conceive, if there is an abnormality, now is the time to correct it in preparation for getting pregnant. The same is true for infectious diseases (like HIV and Hepatitis) which we test for in both the male and female patient before achieving a pregnancy.
Genetic Screening
Genetic Screening is recommended that pregnant women presenting for their first visit be offered genetic screening to see if they are carriers for a handful of diseases. If both the mom and dad are carriers for one of these types of diseases, the baby would have a 25% chance of being affected by the disease. Being a carrier for one of these disorders does not impact your health or your ability to conceive. However, we feel it is important to offer the testing prior to pregnancy. If both parents are carriers for the same disease there are ways that we can help them avoid having a sick child. Our center works with a state of the art genetics laboratory that, in addition to the handful of recommended disorders, can check for over 300 different genetic diseases.
Carrier Screening & Preimplantation Genetic Diagnosis (PGD)
 It is now recommended to offer genetic screening to all couples considering pregnancy. In this circumstance, genetic screening refers to looking for mutations that couples may carry that together could give rise to a child with a genetic disorder. These types of disorders require the child to inherit two copies of the gene, one from their mother and one from their father. By testing for these types of genes before pregnancy we can identify couples who may be at risk for having a child affected by one of these disorders.
It is now recommended to offer genetic screening to all couples considering pregnancy. In this circumstance, genetic screening refers to looking for mutations that couples may carry that together could give rise to a child with a genetic disorder. These types of disorders require the child to inherit two copies of the gene, one from their mother and one from their father. By testing for these types of genes before pregnancy we can identify couples who may be at risk for having a child affected by one of these disorders.
If a couple is found to be at risk for a genetic disorder, this usually means that both the male and the female carry a genetic mutation that will only cause a disease if the child inherits the gene from both mother and father. Armed with the knowledge about the mutation and using the advanced technologies available to us, we can now nearly eliminate the possibility of having a child affected by that genetic disorder.
Working together with our colleagues at genetic laboratories, we would develop probes to the specific gene in question. Then by performing IVF, the embryos are biopsied and a few cells from each embryo are sent to the genetics laboratory. The probe is then used to identify which embryos are not affected by the gene and therefore should be used for transfer. This technique, called Preimplantation Genetic Diagnosis (PGD) has been used to prevent hundreds of different genetic disorders.
Preimplantation Genetic Screening (PGS)
Unlike carrier screening and PGD, PGS looks at the chromosome content of each embryo. A healthy person is born with 46 chromosomes, 23 that they inherited from their mother and 23 from their father. A portion of all embryos will have too many or too few chromosomes, usually as a result of decreasing egg quality as women age. These abnormal embryos will either not implant, or rarely end in an early miscarriage, or even rarer develop into a child that may have a chromosomal disorder such as Down Syndrome (an extra copy of chromosome 21) or Turners Syndrome (a missing copy of the X chromosome). When a couple does IVF they have the option of utilizing PGS, where the are biopsied and a small number of cells sent to a genetics laboratory where they can analyze the chromosome content of each embryo. This allows us to select the embryo/s that will have the highest chance of a leading to a healthy baby.